3 results
A tale of excess: the curious case of the woman with 1447 emergency visits
- M. Sagué Vilavella, A. Giménez Palomo, A. Àvila-Parcet, T. Fernández Plaza, L. Navarro Cortés, G. Oretega Hernández, M. Pons Cabrera, L. Tardón Senabre, M. Vázquez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S286
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Frequent attenders to emergency services are challenging and costly. We report the case of a woman in her mid-twenties who stands out for a total of 1447 emergency visits.
ObjectivesOur primary objective was to describe the emergency visits of our patient. Secondary objectives were to assess her use of other healthcare services and to calculate her health expenditure.
MethodsThis is a clinical case report. We reviewed the patient’s electronic medical records for sociodemographic and clinical data. We obtained detailed information of psychiatric ED visits (length, most frequent times and days) regarding the second most-visited hospital. We assessed the efficacy of hospitalizations in reducing ED visits with a paired samples t Test, comparing the number of visits 30 days pre- and post-hospitalization. We estimated the health expenditure using the regional public health system prices, including three direct costs: emergency visits, hospitalizations and ambulance transportation. We obtained written informed consent from the patient’s legal guardian.
ResultsA 26-year-old woman from Barcelona (Catalonia, Spain), diagnosed with mild intellectual disability, made 1447 emergency visits between 2009 and 2021 (figure 1). 946 visits (65%) took place in psychiatric emergency departments (EDs), whilst 353 (24%) in non-psychiatric EDs and 148 (10%) in urgent primary care. She attended 24 hospitals (ranking number one the closest to the patient’s home, with 387 visits) and seven primary care centers, distributed across 17 cities in Catalonia. Most visits were self-referred, being the main presenting problems anxiety and instrumental suicidal behaviour. Saturday was her favorite day for hospital visits (24,1%), while she seeked care on Tuesdays much less often (4.5%). She made 73.5% of consultations between 1pm and 6pm, with a median length per visit of 2.8 hours (range 0.33-20.9 hours). Regarding other therapeutic approaches, she attended day hospitals, psychiatric rehabilitation programs and family therapy, among others (figure 2), for which she showed low adherence and scarce benefit. She had ten acute hospitalizations, interventions that did not reduce ED visits (t=-0.9835, p=0.36). Health expenditure reached 410.035€.
Image:
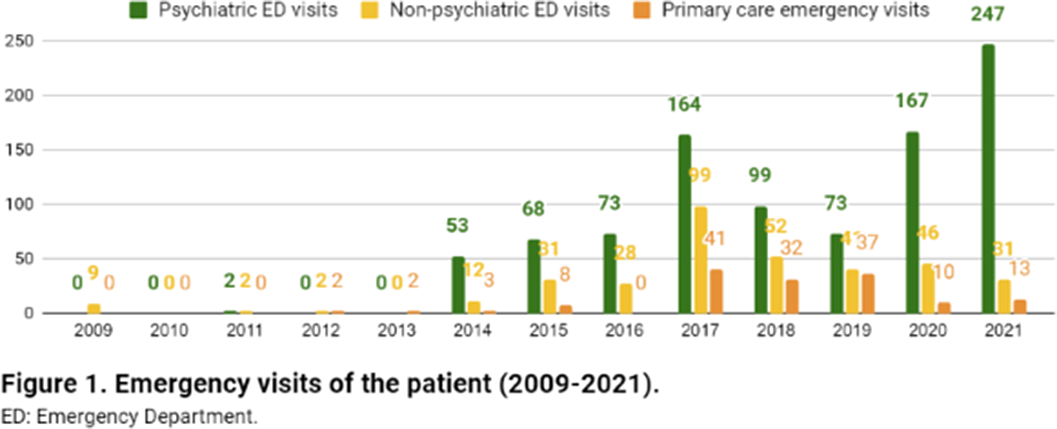
Image 2:
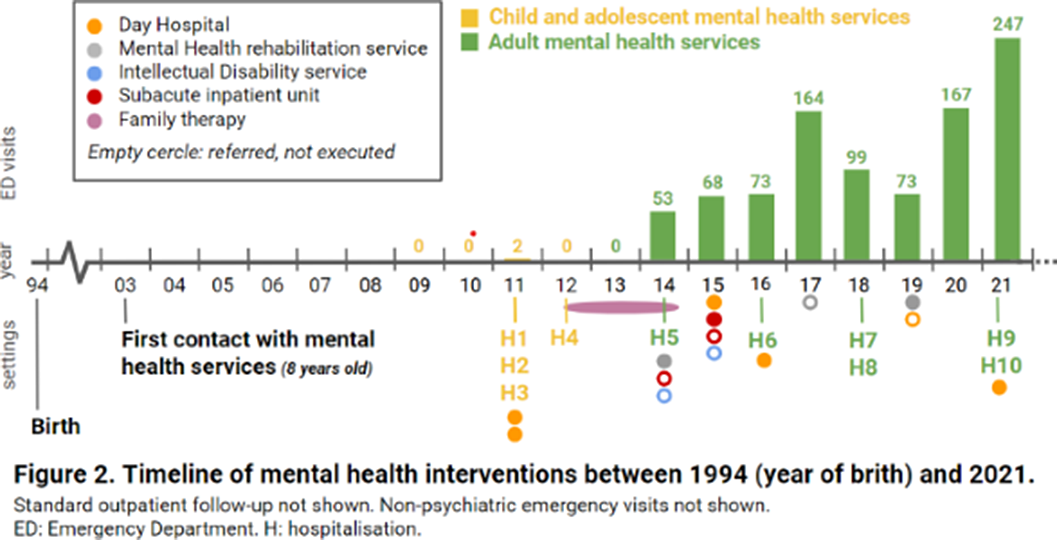 Conclusions
ConclusionsThe most common definition of frequent attendance is a patient who has five or more visits per year. Many times, but not always, repeat visits are also inappropriate. The case we report is a grotesque example of both frequent and inappropriate attendance, which has been resistant to all kinds of interventions and has quality-of-care, financial and ethical implications. As of today, it is still a pending case. Maybe it is worth considering residential treatment?
Disclosure of InterestNone Declared
A family history of suicide in bipolar disorders: powerful, powerless
- M. Sagué Vilavella, G. Fico, G. Anmella, A. Giménez, M. Gómez Ramiro, M. T. Pons Cabrera, S. Madero, A. Murru, E. Vieta
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S387
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
When completing the medical record of a patient with bipolar disoder (BD), hardly anything is more impacting than a family history of completed suicide (FHS). In fact, FHS is a main risk factor for personal suicide attempts and death in this population. There are few modifiable protective factors against suicide in BD, such as lithium treatment and absence of substance abuse.
ObjectivesWe aimed to explore the relationship between a FHS and clinical characteristics in patients with BD. Given the impact that FHS has on the individual and on healthcare professionals, we hypothesized that it would modify behaviors towards a higher prevalence of the modifiable protective factors against suicide, namely more treatment with lithium and less drug addiction.
MethodsThis is a cross-sectional study that included all patients with BD that were followed up in a specialised unit between 1998 and 2020. Only subjects with complete information on FHS were retained for the analysis. We assessed sociodemographic and clinical data and described it with measures of frequency, central tendency and dispersion. Differences between subjects with and without FHS were calculated with χ², Fisher’s exact test and Student’s t-test as appropriate. We set the significance level at p≤0.05. All tests were two-tailed.
ResultsThe sample consisted of 480 subjects with a mean age of 45.9 years (standard deviation 14.4, range 18-88), of which 54.4% (n=261) were women. 69.2% (n=332) had a diagnosis of BD type I and 30.8% (n=148) of BD type II. 77 subjects (16%) had a FHS. Regarding differences between groups, those with relatives who had committed suicide did not show statistically significant differences in terms of sociodemographic variables (age, gender, civil status, employment) or key clinical features (type of BD, illness duration, psychotic features, predominant polarity, rapid cycling, number of lifetime manic and depressive episodes, comorbid personality disorder), neither did they have a higher use of lithium (55.8% vs 59.3%, p=0.572) nor lower substance use disorder (10.9% vs 15.5%, p=0.34). Predictably, people with FHS had a higher prevalence of family history of mental and affective disorders (96.1% vs 70.9%, p<0.001; 86.3% vs 56.3%, p<0.001) and of stressful life events (71.6% vs 58.9%, p=0.05). Personal lifetime suicide attempts also tended to be higher (36.4% vs 26.7%, p=0.088).
ConclusionsContrary to our hypothesis, in our sample of subjects with BD a FHS was not associated with a higher prevalence of the modifiable protective factors against suicide. Therefore, although suicide has a major impact both in families and healthcare professionals, our results suggest it does not modify attitudes towards prevention in a real-life scenario. The main limitation of our study is its cross-sectional design, which does not allow for causal inference. In conclusion, there is room for improvement in the fight against suicide.
Disclosure of InterestNone Declared
Bipolar disorders and suicide: stumbling twice with the same stone?
- M. Sagué-Vilavella, G. Fico, G. Anmella, A. Giménez-Palomo, M. Gómez-Ramiro, M. Pons Cabrera, S. Madero, E. Vieta, A. Murru
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S222-S223
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicide is the most terrible outcome of bipolar disorders (BD). It impacts families and healthcare professionals deeply. Family history of suicide (FHS) is one of its main risk factors, whereas lithium treatment and absence of substance use disorders (SUD) are two of its few modifiable protective factors.
ObjectivesTo explore the relationship between FHS and clinical characteristics in BD. We hypothesized that FHS would be associated with less SUD, higher rates of lithium treatment and shorter duration of untreated illness (DUI).
MethodsCross-sectional analysis of subjects with BD followed-up in a specialised outpatient unit (Barcelona, October’08-March’18). We described data with measures of frequency, central tendency and dispersion, and we used χ², Fisher’s test and t-tests for comparisons.
ResultsThe sample consisted of 83 subjects, 56.6% males, mean age 41.9 years (SD 12.7). 74.7% (n=62) had a diagnosis of BD-I and 25.3% (n=21) of BD-II. 11 subjects (13.3%) had FHS. Those with FHS did not show significant differences in sociodemographic data, DUI (58.5+/-60.4 vs 38.19+/-84.9 months, p=0.341), lithium use (72.7% vs 73.6%, p=0.95) or SUD (27.3% vs 23.6%, p=0.79). There were differences in terms of lifetime suicide attempts (54.5% vs 20.8%, p=0.026), family history of mental disorders (100% vs 69.4%, n=0.032).
ConclusionsContrary to our hypothesis, FHS was not associated with the modifiable protective factors against suicide (namely, less SUD and more lithium prescription). Similarly, we did not find an association with earlier access to mental health services at symptom onset (DUP as proxy). Therefore, our results suggest FHS does not modify attitudes towards prevention.
DisclosureNo significant relationships.





